Despite increased recognition of MOGAD as a distinct disease and the availability of sensitive methods of MOG antibody testing, diagnostic challenges remain. 1988 130(3):443–454.Myelin oligodendrocyte glycoprotein antibody-associated disease (MOGAD) is a rare demyelinating disorder of the central nervous system. Augmentation of demyelination in rat acute allergic encephalomyelitis by circulating mouse monoclonal antibodies directed against a myelin/oligodendrocyte glycoprotein. Antibody responses in chronic relapsing experimental allergic encephalomyelitis: correlation of serum demyelinating activity with antibody titre to the myelin/oligodendrocyte glycoprotein (MOG) J Neuroimmunol. The structure and function of myelin oligodendrocyte glycoprotein. Myelin oligodendrocyte glycoprotein: a novel candidate autoantigen in multiple sclerosis. A monoclonal antibody against a myelin oligodendrocyte glycoprotein induces relapses and demyelination in central nervous system autoimmune disease. CNS central nervous system, MOG-AD myelin oligodendrocyte glycoprotein antibody disease, MOG myelin oligodendrocyte glycoprotein, IV intravenous While it is reasonable and common practice to treat relapsing patients with long-term immunosuppression, the duration of disease-modifying treatment remains uncertain. If a lack of response to immunosuppressants is demonstrated or a disabling recurrence of the disease occurs after cessation of oral steroids, it is appropriate to consider monoclonal antibodies. 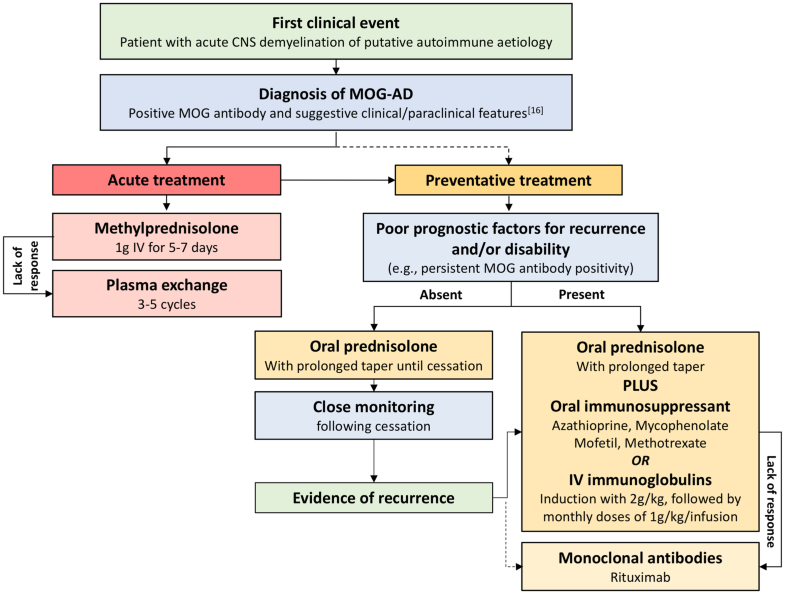
On this basis, treatment may require a prolonged taper with oral steroids (advised in the absence of poor prognostic factors) or the use of oral immunosuppressants or intravenous immunoglobulins along with oral steroids (advised as first choice in the presence of poor prognostic factors). The choice of the disease-modifying agent should be guided by the presence or absence of poor prognostic factors for recurrence and/or disability. After diagnosis and, usually, acute treatment, initiation of disease-modifying therapy is advised. Acute treatment with steroids and, if needed, subsequent plasma exchange are advised as soon as possible after an acute event. This proposed therapeutic management of MOG-AD is based on current evidence. Randomised control trials are limited, but observational open-label experience suggests a role for high-dose steroids and plasma exchange in the treatment of acute attacks, and for immunosuppressive therapies, such as steroids, oral immunosuppressants and rituximab as maintenance treatment.Ĭerebrospinal fluid (CSF) MRI Multiple sclerosis (MS) Myelin oligodendrocyte glycoprotein (MOG) antibodies Neuromyelitis optica (NMO) Optic neuritis (ON). Cerebrospinal fluid oligoclonal bands are uncommon. MRI characteristics can help in differentiating MOG-AD from other neuroinflammatory disorders, including multiple sclerosis and neuromyelitis optica. To avoid misdiagnosis, MOG antibody testing should be undertaken in selected cases presenting clinical and paraclinical features that are felt to be in keeping with MOG-AD, using a validated cell-based assay. Recent advances in MOG antibody testing offer improved sensitivity and specificity. Residual disability develops in 50-80% of patients, with transverse myelitis at onset being the most significant predictor of long-term outcome. Disease course can be either monophasic or relapsing, with subsequent relapses most commonly involving the optic nerve. Although no age group is exempt, median age of onset is within the fourth decade of life, with optic neuritis being the most frequent presenting phenotype. Myelin oligodendrocyte glycoprotein (MOG) antibody disease (MOG-AD) is now recognised as a nosological entity with specific clinical and paraclinical features to aid early diagnosis. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
